Human Anatomy and Physiology : Introduction to the Reproductive System
Introduction to the Reproductive System
The major function of the reproductive system is to ensure survival of the species. Other systems in the body, such as the endocrine and urinary systems, work continuously to maintain homeostasis for survival of the individual. An individual may live a long, healthy, and happy life without producing offspring, but if the species is to continue, at least some individuals must produce offspring.
Within the context of producing offspring, the reproductive system has four functions:
- To produce egg and sperm cells
- To transport and sustain these cells
- To nurture the developing offspring
- To produce hormones
These functions are divided between the primary and secondary, or accessory, reproductive organs. The primary reproductive organs, or gonads, consist of the ovaries and testes. These organs are responsible for producing the egg and sperm cells gametes), and hormones. These hormones function in the maturation of the reproductive system, the development of sexual characteristics, and regulation of the normal physiology of the reproductive system. All other organs, ducts, and glands in the reproductive system are considered secondary, or accessory, reproductive organs. These structures transport and sustain the gametes and nurture the developing offspring.
- Male Reproductive System
The male reproductive system, like that of the female, consists of those organs whose function is to produce a new individual, i.e., to accomplish reproduction. This system consists of a pair of testes and a network of excretory ducts (epididymis, ductus deferens (vas deferens), and ejaculatory ducts), seminal vesicles, the prostate, the bulbourethral glands, and the penis.
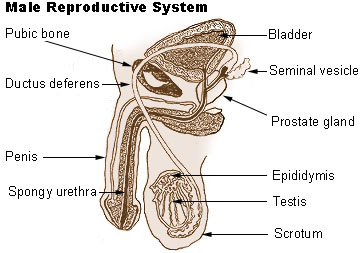
Testes
The male gonads, testes or testicles, begin their development high in the abdominal cavity, near the kidneys. During the last two months before birth, or shortly after birth, they descend through the inguinal canal into the scrotum, a pouch that extends below the abdomen, posterior to the penis. Although this location of the testes, outside the abdominal cavity, may seem to make them vulnerable to injury, it provides a temperature about 3° C below normal body temperature. This lower temperature is necessary for the production of viable sperm.
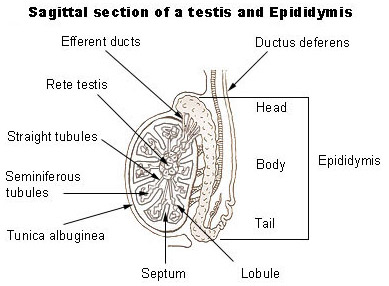
The scrotum consists of skin and subcutaneous tissue. A vertical septum, or partition, of subcutaneous tissue in the center divides it into two parts, each containing one testis. Smooth muscle fibers, called the dartos muscle, in the subcutaneous tissue contract to give the scrotum its wrinkled appearance. When these fibers are relaxed, the scrotum is smooth. Another muscle, the cremaster muscle, consists of skeletal muscle fibers and controls the position of the scrotum and testes. When it is cold or a man is sexually aroused, this muscle contracts to pull the testes closer to the body for warmth.
Structure
Each testis is an oval structure about 5 cm long and 3 cm in diameter. A tough, white fibrous connective tissue capsule, the tunica albuginea, surrounds each testis and extends inward to form septa that partition the organ into lobules. There are about 250 lobules in each testis. Each lobule contains 1 to 4 highly coiled seminiferous tubules that converge to form a single straight tubule, which leads into the rete testis. Short efferent ducts exit the testes. Interstitial cells (cells of Leydig), which produce male sex hormones, are located between the seminiferous tubules within a lobule.
Spermatogenesis
Sperm are produced by spermatogenesis within the seminiferous tubules. A transverse section of a seminiferous tubule shows that it is packed with cells in various stages of development. Interspersed with these cells, there are large cells that extend from the periphery of the tubule to the lumen. These large cells are the supporting, or sustentacular cells (Sertoli's cells), which support and nourish the other cells.
Early in embryonic development, primordial germ cells enter the testes and differentiate into spermatogonia, immature cells that remain dormant until puberty. Spermatogonia are diploid cells, each with 46 chromosomes (23 pairs) located around the periphery of the seminiferous tubules. At puberty, hormones stimulate these cells to begin dividing by mitosis. Some of the daughter cells produced by mitosis remain at the periphery as spermatogonia. Others are pushed toward the lumen, undergo some changes, and become primary spermatocytes. Because they are produced by mitosis, primary spermatocytes, like spermatogonia, are diploid and have 46 chromosomes.
Each primary spermatocytes goes through the first meiotic division, meiosis I, to produce two secondary spermatocytes, each with 23 chromosomes (haploid). Just prior to this division, the genetic material is replicated so that each chromosome consists of two strands, called chromatids, that are joined by a centromere. During meiosis I, one chromosome, consisting of two chromatids, goes to each secondary spermatocyte. In the second meiotic division, meiosis II, each secondary spermatocyte divides to produce two spermatids. There is no replication of genetic material in this division, but the centromere divides so that a single-stranded chromatid goes to each cell. As a result of the two meiotic divisions, each primary spermatocyte produces four spermatids. During spermatogenesis there are two cellular divisions, but only one replication of DNA so that each spermatid has 23 chromosomes (haploid), one from each pair in the original primary spermatocyte. Each successive stage in spermatogenesis is pushed toward the center of the tubule so that the more immature cells are at the periphery and the more differentiated cells are nearer the center.
Spermatogenesis (and oogenesis in the female) differs from mitosis because the resulting cells have only half the number of chromosomes as the original cell. When the sperm cell nucleus unites with an egg cell nucleus, the full number of chromosomes is restored. If sperm and egg cells were produced by mitosis, then each successive generation would have twice the number of chromosomes as the preceding one.
The final step in the development of sperm is called spermiogenesis. In this process, the spermatids formed from spermatogenesis become mature spermatozoa, or sperm. The mature sperm cell has a head, midpiece, and tail. The head, also called the nuclear region, contains the 23 chromosomes surrounded by a nuclear membrane. The tip of the head is covered by an acrosome, which contains enzymes that help the sperm penetrate the female gamete. The midpiece, metabolic region, contains mitochondria that provide adenosine triphosphate (ATP). The tail or locomotor region, uses a typical flagellum for locomotion. The sperm are released into the lumen of the seminiferous tubule and leave the testes. They then enter the epididymis where they undergo their final maturation and become capable of fertilizing a female gamete.
Sperm production begins at puberty and continues throughout the life of a male. The entire process, beginning with a primary spermatocyte, takes about 74 days. After ejaculation, the sperm can live for about 48 hours in the female reproductive tract.
Duct System
Sperm cells pass through a series of ducts to reach the outside of the body. After they leave the testes, the sperm passes through the epididymis, ductus deferens, ejaculatory duct, and urethra.
Epididymis
Sperm leave the testes through a series of efferent ducts that enter the epididymis. Each epididymis is a long (about 6 meters) tube that is tightly coiled to form a comma-shaped organ located along the superior and posterior margins of the testes. When the sperm leave the testes, they are immature and incapable of fertilizing ova. They complete their maturation process and become fertile as they move through the epididymis. Mature sperm are stored in the lower portion, or tail, of the epididymis.
Ductus Deferens
The ductus deferens, also called vas deferens, is a fibromuscular tube that is continuous ( or contiguous) with the epididymis. It begins at the bottom (tail) of the epididymis then turns sharply upward along the posterior margin of the testes. The ductus deferens enters the abdominopelvic cavity through the inguinal canal and passes along the lateral pelvic wall. It crosses over the ureter and posterior portion of the urinary bladder, and then descends along the posterior wall of the bladder toward the prostate gland. Just before it reaches the prostate gland, each ductus deferens enlarges to form an ampulla. Sperm are stored in the proximal portion of the ductus deferens, near the epididymis, and peristaltic movements propel the sperm through the tube.
The proximal portion of the ductus deferens is a component of the spermatic cord, which contains vascular and neural structures that supply the testes. The spermatic cord contains the ductus deferens, testicular artery and veins, lymph vessels, testicular nerve, cremaster muscle that elevates the testes for warmth and at times of sexual stimulation, and a connective tissue covering.
Ejaculatory Duct
Each ductus deferens, at the ampulla, joins the duct from the adjacent seminal vesicle (one of the accessory glands) to form a short ejaculatory duct. Each ejaculatory duct passes through the prostate gland and empties into the urethra.
Urethra
The urethra extends from the urinary bladder to the external urethral orifice at the tip of the penis. It is a passageway for sperm and fluids from the reproductive system and urine from the urinary system. While reproductive fluids are passing through the urethra, sphincters contract tightly to keep urine from entering the urethra.
The male urethra is divided into three regions. The prostatic urethra is the proximal portion that passes through the prostate gland. It receives the ejaculatory duct, which contains sperm and secretions from the seminal vesicles, and numerous ducts from the prostate glands. The next portion, the membranous urethra, is a short region that passes through the pelvic floor. The longest portion is the penile urethra (also called spongy urethra or cavernous urethra), which extends the length of the penis and opens to the outside at the external urethral orifice. The ducts from the bulbourethral glands open into the penile urethra.
Accessory Glands
The accessory glands of the male reproductive system are the seminal vesicles, prostate gland, and the bulbourethral glands. These glands secrete fluids that enter the urethra.
Seminal Vesicles
The paired seminal vesicles are saccular glands posterior to the urinary bladder. Each gland has a short duct that joins with the ductus deferens at the ampulla to form an ejaculatory duct, which then empties into the urethra. The fluid from the seminal vesicles is viscous and contains fructose, which provides an energy source for the sperm; prostaglandins, which contribute to the mobility and viability of the sperm; and proteins that cause slight coagulation reactions in the semen after ejaculation.
Prostate
The prostate gland is a firm, dense structure that is located just inferior to the urinary bladder. It is about the size of a walnut and encircles the urethra as it leaves the urinary bladder. Numerous short ducts from the substance of the prostate gland empty into the prostatic urethra. The secretions of the prostate are thin, milky colored, and alkaline. They function to enhance the motility of the sperm.
Bulbourethral Glands
The paired bulbourethral (Cowper's) glands are small, about the size of a pea, and located near the base of the penis. A short duct from each gland enters the proximal end of the penile urethra. In response to sexual stimulation, the bulbourethral glands secrete an alkaline mucus-like fluid. This fluid neutralizes the acidity of the urine residue in the urethra, helps to neutralize the acidity of the vagina, and provides some lubrication for the tip of the penis during intercourse.
Seminal Fluid
Seminal fluid, or semen, is a slightly alkaline mixture of sperm cells and secretions from the accessory glands. Secretions from the seminal vesicles make up about 60 percent of the volume of the semen, with most of the remainder coming from the prostate gland. The sperm and secretions from the bulbourethral gland contribute only a small volume.
The volume of semen in a single ejaculation may vary from 1.5 to 6.0 ml. There are usually between 50 to 150 million sperm per milliliter of semen. Sperm counts below 10 to 20 million per milliliter usually present fertility problems. Although only one sperm actually penetrates and fertilizes the ovum, it takes several million sperm in an ejaculation to ensure that fertilization will take place.
Penis
The penis, the male copulatory organ, is a cylindrical pendant organ located anterior to the scrotum and functions to transfer sperm to the vagina. The penis consists of three columns of erectile tissue that are wrapped in connective tissue and covered with skin. The two dorsal columns are the corpora cavernosa. The single, midline ventral column surrounds the urethra and is called the corpus spongiosum.
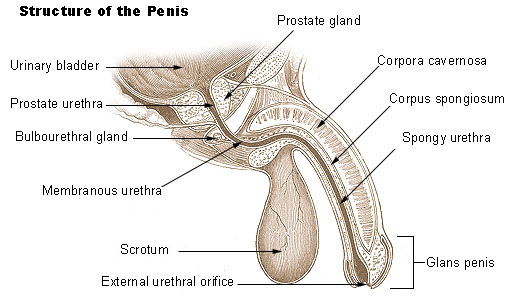
The penis has a root, body (shaft), and glans penis. The root of the penis attaches it to the pubic arch, and the body is the visible, pendant portion. The corpus spongiosum expands at the distal end to form the glans penis. The urethra, which extends throughout the length of the corpus spongiosum, opens through the external urethral orifice at the tip of the glans penis. A loose fold of skin, called the prepuce, or foreskin, covers the glans penis.
Male Sexual Response and Hormonal Control
The male sexual response includes erection and orgasm accompanied by ejaculation of semen. Orgasm is followed by a variable time period during which it is not possible to achieve another erection.
Three hormones are the principle regulators of the male reproductive system: follicle-stimulating hormone (FSH) stimulates spermatogenesis; luteinizing hormone (LH) stimulates the production of testosterone; and testosterone stimulates the development of male secondary sex characteristics and spermatogenesis.
- Female Reproductive System
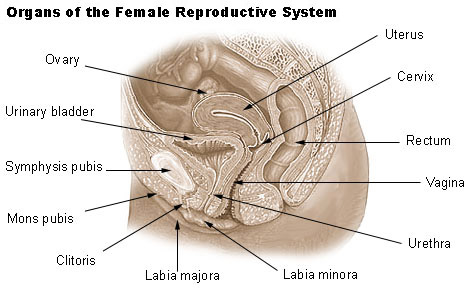
The organs of the female reproductive system produce and sustain the female sex cells (egg cells or ova), transport these cells to a site where they may be fertilized by sperm, provide a favorable environment for the developing fetus, move the fetus to the outside at the end of the development period, and produce the female sex hormones. The female reproductive system includes the ovaries, Fallopian tubes, uterus, vagina, accessory glands, and external genital organs.
- Ovaries
- Genital Tract
- External Genitalia
- Female Sexual Response and Hormonal Control
- Mammary Glands
Ovaries
The primary female reproductive organs, or gonads, are the two ovaries. Each ovary is a solid, ovoid structure about the size and shape of an almond, about 3.5 cm in length, 2 cm wide, and 1 cm thick. The ovaries are located in shallow depressions, called ovarian fossae, one on each side of the uterus, in the lateral walls of the pelvic cavity. They are held loosely in place by peritoneal ligaments.
Structure
The ovaries are covered on the outside by a layer of simple cuboidal epithelium called germinal (ovarian) epithelium. This is actually the visceral peritoneum that envelops the ovaries. Underneath this layer is a dense connective tissue capsule, the tunica albuginea. The substance of the ovaries is distinctly divided into an outer cortex and an inner medulla. The cortex appears more dense and granular due to the presence of numerous ovarian follicles in various stages of development. Each of the follicles contains an oocyte, a female germ cell. The medulla is a loose connective tissue with abundant blood vessels, lymphatic vessels, and nerve fibers.
Oogenesis
Female sex cells, or gametes, develop in the ovaries by a form of meiosis called oogenesis. The sequence of events in oogenesis is similar to the sequence in spermatogenesis, but the timing and final result are different. Early in fetal development, primitive germ cells in the ovaries differentiate into oogonia. These divide rapidly to form thousands of cells, still called oogonia, which have a full complement of 46 (23 pairs) chromosomes. Oogonia then enter a growth phase, enlarge, and become primary oocytes. The diploid (46 chromosomes) primary oocytes replicate their DNA and begin the first meiotic division, but the process stops in prophase and the cells remain in this suspended state until puberty. Many of the primary oocytes degenerate before birth, but even with this decline, the two ovaries together contain approximately 700,000 oocytes at birth. This is the lifetime supply, and no more will develop. This is quite different than the male in which spermatogonia and primary spermatocytes continue to be produced throughout the reproductive lifetime. By puberty the number of primary oocytes has further declined to about 400,000.
Beginning at puberty, under the influence of follicle-stimulating hormone, several primary oocytes start to grow again each month. One of the primary oocytes seems to outgrow the others and it resumes meiosis I. The other cells degenerate. The large cell undergoes an unequal division so that nearly all the cytoplasm, organelles, and half the chromosomes go to one cell, which becomes a secondary oocyte. The remaining half of the chromosomes go to a smaller cell called the first polar body. The secondary oocyte begins the second meiotic division, but the process stops in metaphase. At this point ovulation occurs. If fertilization occurs, meiosis II continues. Again this is an unequal division with all of the cytoplasm going to the ovum, which has 23 single-stranded chromosome. The smaller cell from this division is a second polar body. The first polar body also usually divides in meiosis I to produce two even smaller polar bodies. If fertilization does not occur, the second meiotic division is never completed and the secondary oocyte degenerates. Here again there are obvious differences between the male and female. In spermatogenesis, four functional sperm develop from each primary spermatocyte. In oogenesis, only one functional fertilizable cell develops from a primary oocyte. The other three cells are polar bodies and they degenerate.
Ovarian Follicle Development
An ovarian follicle consists of a developing oocyte surrounded by one or more layers of cells called follicular cells. At the same time that the oocyte is progressing through meiosis, corresponding changes are taking place in the follicular cells. Primordial follicles, which consist of a primary oocyte surrounded by a single layer of flattened cells, develop in the fetus and are the stage that is present in the ovaries at birth and throughout childhood.
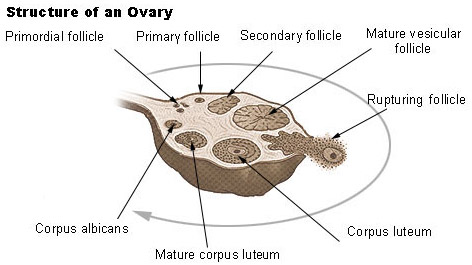
Beginning at puberty, follicle-stimulating hormone stimulates changes in the primordial follicles. The follicular cells become cuboidal, the primary oocyte enlarges, and it is now a primary follicle. The follicles continue to grow under the influence of follicle-stimulating hormone, and the follicular cells proliferate to form several layers of granulose cells around the primary oocyte. Most of these primary follicles degenerate along with the primary oocytes within them, but usually one continues to develop each month. The granulosa cells start secreting estrogen and a cavity, or antrum, forms within the follicle. When the antrum starts to develop, the follicle becomes a secondary follicle. The granulose cells also secrete a glycoprotein substance that forms a clear membrane, the zona pellucida, around the oocyte. After about 10 days of growth the follicle is a mature vesicular (graafian) follicle, which forms a "blister" on the surface of the ovary and contains a secondary oocyte ready for ovulation.
Ovulation
Ovulation, prompted by luteinizing hormone from the anterior pituitary, occurs when the mature follicle at the surface of the ovary ruptures and releases the secondary oocyte into the peritoneal cavity. The ovulated secondary oocyte, ready for fertilization is still surrounded by the zona pellucida and a few layers of cells called the corona radiata. If it is not fertilized, the secondary oocyte degenerates in a couple of days. If a sperm passes through the corona radiata and zona pellucida and enters the cytoplasm of the secondary oocyte, the second meiotic division resumes to form a polar body and a mature ovum
After ovulation and in response to luteinizing hormone, the portion of the follicle that remains in the ovary enlarges and is transformed into a corpus luteum. The corpus luteum is a glandular structure that secretes progesterone and some estrogen. Its fate depends on whether fertilization occurs. If fertilization does not take place, the corpus luteum remains functional for about 10 days; then it begins to degenerate into a corpus albicans, which is primarily scar tissue, and its hormone output ceases. If fertilization occurs, the corpus luteum persists and continues its hormone functions until the placenta develops sufficiently to secrete the necessary hormones. Again, the corpus luteum ultimately degenerates into corpus albicans, but it remains functional for a longer period of time.
Genital Tract
Fallopian Tubes
There are two uterine tubes, also called Fallopian tubes or oviducts. There is one tube associated with each ovary. The end of the tube near the ovary expands to form a funnel-shaped infundibulum, which is surrounded by fingerlike extensions called fimbriae. Because there is no direct connection between the infundibulum and the ovary, the oocyte enters the peritoneal cavity before it enters the Fallopian tube. At the time of ovulation, the fimbriae increase their activity and create currents in the peritoneal fluid that help propel the oocyte into the Fallopian tube. Once inside the Fallopian tube, the oocyte is moved along by the rhythmic beating of cilia on the epithelial lining and by peristaltic action of the smooth muscle in the wall of the tube. The journey through the Fallopian tube takes about 7 days. Because the oocyte is fertile for only 24 to 48 hours, fertilization usually occurs in the Fallopian tube.
Uterus
The uterus is a muscular organ that receives the fertilized oocyte and provides an appropriate environment for the developing fetus. Before the first pregnancy, the uterus is about the size and shape of a pear, with the narrow portion directed inferiorly. After childbirth, the uterus is usually larger, then regresses after menopause.
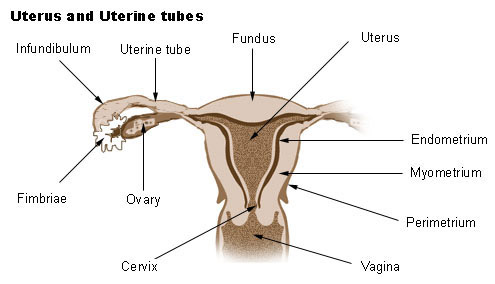
The uterus is lined with the endometrium. The stratum functionale of the endometrium sloughs off during menstruation. The deeper stratum basale provides the foundation for rebuilding the stratum functionale.
Vagina
The vagina is a fibromuscular tube, about 10 cm long, that extends from the cervix of the uterus to the outside. It is located between the rectum and the urinary bladder. Because the vagina is tilted posteriorly as it ascends and the cervix is tilted anteriorly, the cervix projects into the vagina at nearly a right angle. The vagina serves as a passageway for menstrual flow, receives the erect penis during intercourse, and is the birth canal during childbirth.
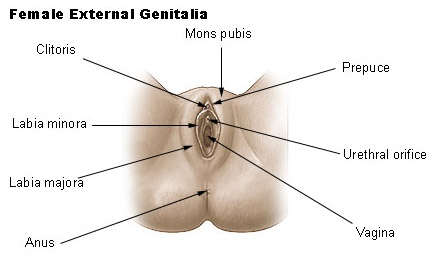
External Genitalia
The external genitalia are the accessory structures of the female reproductive system that are external to the vagina. They are also referred to as the vulva or pudendum. The external genitalia include the labia majora, mons pubis, labia minora, clitoris, and glands within the vestibule.
The clitoris is an erectile organ, similar to the male penis, that responds to sexual stimulation. Posterior to the clitoris, the urethra, vagina, paraurethral glands and greater vestibular glands open into the vestibule.
Female Sexual Response & Hormone Control
The female sexual response includes arousal and orgasm, but there is no ejaculation. A woman may become pregnant without having an orgasm.
Follicle-stimulating hormone, luteinizing hormone, estrogen, and progesterone have major roles in regulating the functions of the female reproductive system.
At puberty, when the ovaries and uterus are mature enough to respond to hormonal stimulation, certain stimuli cause the hypothalamus to start secreting gonadotropin-releasing hormone. This hormone enters the blood and goes to the anterior pituitary gland where it stimulates the secretion of follicle-stimulating hormone and luteinizing hormone. These hormones, in turn, affect the ovaries and uterus and the monthly cycles begin. A woman's reproductive cycles last from menarche to menopause.
The monthly ovarian cycle begins with the follicle development during the follicular phase, continues with ovulation during the ovulatory phase, and concludes with the development and regression of the corpus luteum during the luteal phase.
The uterine cycle takes place simultaneously with the ovarian cycle. The uterine cycle begins with menstruation during the menstrual phase, continues with repair of the endometrium during the proliferative phase, and ends with the growth of glands and blood vessels during the secretory phase.
Menopause occurs when a woman's reproductive cycles stop. This period is marked by decreased levels of ovarian hormones and increased levels of pituitary follicle-stimulating hormone and luteinizing hormone. The changing hormone levels are responsible for the symptoms associated with menopause.
Mammary Glands
Functionally, the mammary glands produce milk; structurally, they are modified sweat glands. Mammary glands, which are located in the breast overlying the pectoralis major muscles, are present in both sexes, but usually are functional only in the female.
Externally, each breast has a raised nipple, which is surrounded by a circular pigmented area called the areola. The nipples are sensitive to touch, due to the fact that they contain smooth muscle that contracts and causes them to become erect in response to stimulation.
Internally, the adult female breast contains 15 to 20 lobes of glandular tissue that radiate around the nipple. The lobes are separated by connective tissue and adipose. The connective tissue helps support the breast. Some bands of connective tissue, called suspensory (Cooper's) ligaments, extend through the breast from the skin to the underlying muscles. The amount and distribution of the adipose tissue determines the size and shape of the breast. Each lobe consists of lobules that contain the glandular units. A lactiferous duct collects the milk from the lobules within each lobe and carries it to the nipple. Just before the nipple, the lactiferous duct enlarges to form a lactiferous sinus (ampulla), which serves as a reservoir for milk. After the sinus, the duct again narrows and each duct opens independently on the surface of the nipple.
Mammary gland function is regulated by hormones. At puberty, increasing levels of estrogen stimulate the development of glandular tissue in the female breast. Estrogen also causes the breast to increase in size through the accumulation of adipose tissue. Progesterone stimulates the development of the duct system. During pregnancy, these hormones enhance further development of the mammary glands. Prolactin from the anterior pituitary stimulates the production of milk within the glandular tissue, and oxytocin causes the ejection of milk from the glands.
Review: Introduction to the Reproductive System
Here is what we have learned from Introduction to the Reproductive System:
- The four functions of the reproductive system are:
- To produce egg and sperm cells
- To transport and sustain these cells
- To nurture the developing fetus
- To produce hormones
- The primary reproductive organs are the gonads, which produce the gametes and hormones. The secondary, or accessory, structures transport and sustain the gametes and nurture the developing offspring.
- The male reproductive system consists of the testes, duct system, accessory glands, and penis.
- The male gonads are the testes. Their location within the scrotum is necessary for the production of viable sperm.
- The female reproductive system includes the ovaries, uterine tubes, uterus, vagina, accessory glands, and external genital organs.
- The female gonads are the ovaries, which are located on each side of the uterus in the pelvic cavity.
- Estrogen and progesterone stimulate the development of glandular tissue and ducts in the breast. Prolactin stimulates the production of milk, and oxytocin causes the ejection of milk.
Comments
Post a Comment